What is High Frequency Chest Wall Oscillation (HFCWO)?
The problem of clearing the airways of those ill with pulmonary diseases has been a challenge for ages. Typically, coughing to clear obstruction works well for those with normal lung function. However, the immune system and airway mucous clearance mechanisms need to work together to keep our airways clear and free of disease. If one or more of these mechanisms is impaired, then there can be difficulty completely clearing secretions from the airways. This may cause obstruction to our breathing, and respiratory distress. If secretions are not being expelled, We may need intervention to help shake loose the mucous trapped in our lungs when things go wrong. This is where High Frequency Chest Wall Oscillation (HFCWO) may be prescribed.
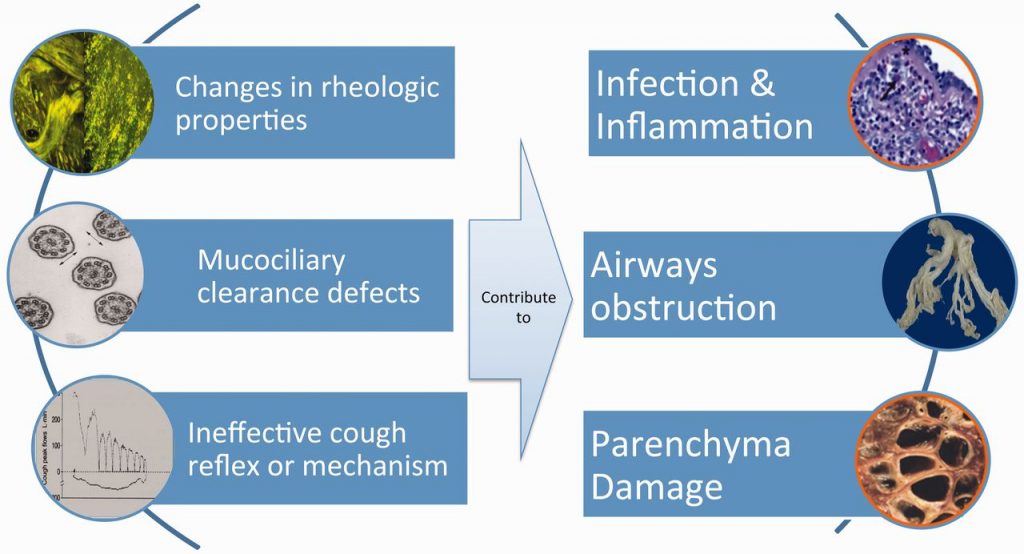
How does HFCWO/HFCWC work?
High-Frequency Oscillation and Compression therapies work through the chest wall itself. Either through manual hand cupping and clapping, or through mechanically transmitted percussive waves, with steady rhythm. This force travels through the airways to shake loose the mucous with shearing forces, to make them easier to cough out. There are handheld percussion devices that can be placed over areas of the chest that the patient can reach. While these devices are helpful, they have their limitations in efficacy. In vest devices, a vest outfitted with several inflatable air pockets applies percussive waves over the lung. However, the necessity of a tight fit to the thorax limits the patient from full expansion of the chest and therefore inhibits maximal alveolar recruitment. Although they are considered helpful in the clearance of sputum and maintenance of clearer airways, the restrictive nature of HFCWC will inhibit lung recruitment as part of their mechanism, limiting the benefits of this mode of therapy[1].
What is the difference between High Frequency Chest Wall Oscillation, and Compression?
High Frequency Chest Wall Oscillation (HFCWO) occurs when 2 forces are sequentially applied to first compress, then expand the chest wall. The term oscillation refers to both a compression, and expansion motion of a surface to either side of a central point. This motion is distinctive from the mode of therapy of chest wall percussion as that mode depresses only inward, with return to baseline. Only devices that are capable of applying both compression and distension of the chest wall can be truly qualified as a chest wall oscillator. The benefit of this intervention is the ability to more effectively attune the frequency of vibration to the quality of sputum for the patient/disease process. This serves to accelerate the liquefaction of the sputum thus allowing easier expectoration. In HFCWO, the device transmits the oscillating wave throughout the thorax and patients often report it to be more comfortable than chest wall percussion or compression. Contrary to what most manufacturers claim, many vest devices are actually delivering high frequency chest wall compressions, not oscillation. Rather than the pull and push motions against the chest of HFCWO, HFCWC squeezes then relies on the chest wall’s natural rebound to return to the starting point.
How do we clear secretions?
External oscillatory effect can be applied to the chest through percussive waves created by chest wall compression or through chest wall oscillation. This transmits to the airways of the patients and creates shearing forces that cause sputum to loosen from the wall of the airways. Hopefully, the loosened sputum will be more affected by the expiratory flow of air in central airways to be expectorated by the patient. These interventions have been used for many years in patients with Cystic Fibrosis, Bronchiectasis and COPD with good effect. However, as pulmonary function worsens in these patients, the capacity for expectoration is compromised by the loss of cough flow.
Indeed, in one study that used vest therapy vs hand cupping and clapping (CCPT) it was noted that tidal volume and pulse oximetry was compromised by post vest therapy [2]. Although the ventilator settings themselves did not change when using vest therapy, the physiologic effects were also evident by the noted increase in mean airway pressure and rapid breathing noted in the patients who used vest therapy compared to those who received CCPT. This makes it clear that even in patients who are actively receiving airway support from positive pressure ventilation, that the restrictive nature of vest therapy on the ability of the chest wall to fully expand is felt and evidenced by measurable changes in the patient’s condition.[3]
How can we get true High Frequency Chest Wall Oscillation without a vest?
BCV (Biphasic Cuirass Ventilation) when applied for secretion clearance support therapy delivers true chest wall oscillation without compromise of FRC (Functional Residual Capacity) . The cuirass covers only the anterior and lateral portions of the thorax and upper abdomen. This allows the patient to sit comfortably in a chair or lie in bed while therapy is administered. As the Biphasic nature of this device does not inhibit chest wall excursion, there is no risk of inducing atelectasis with this intervention, allowing it to be used for more prolonged treatment than chest wall percussors.
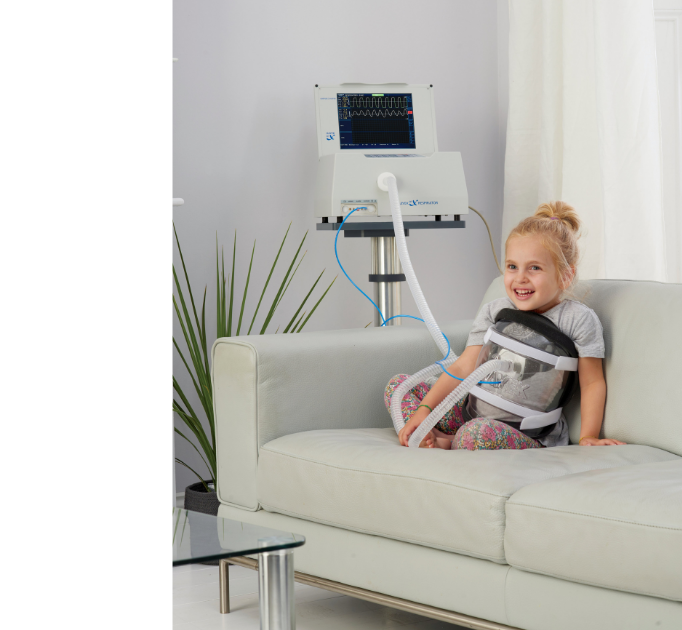
Additionally, the cough assist mechanism employed here that is administered for set periods, in cycle with periods of chest wall oscillation. Cough, assisted by the cuirass works by amplifying the natural cough mechanism of our patient. This can enhance the effectiveness of expectoration efforts of those with normal lung function, as well as supporting improved cough efficacy of those with compromised cough force through loss of pulmonary muscle or lung function.
How does Biphasic Cuirass Ventilation (BCV) support compromised patients?
It is in these compromised patients that BCV distinguishes itself from traditional vest style therapies. In addition to HFCWO, BCV offers a recruitment option in Continuous Negative and a NIV option in the biphasic ventilation settings. It naturally enhances chest wall excursion and opens the lung, while vest therapy naturally restricts it. In those patients with already impaired cough strength, there is little reserve left that can allow for any further compromise. Employment of BCV at any stage of disease is optimal as it will not accelerate any deterioration of lung function. It can also support, and possibly improve the lung function of more advanced disease processes. It would seem that utilizing BCV therapy early in any disease process gives the optimal chance of good pulmonary outcomes with no chance of restricting lung function.
[1]: https://www.hillrom.com/content/dam/hillrom-aem/us/en/marketing/knowledge/product-documentation/white-papers/197151-EN-r1_HFCWO-Airflow_Whitepaper_LR.pdf
[2/3]: https://pubmed.ncbi.nlm.nih.gov/28248854/